Medication and technical errors continue to occur from time to time in anaesthesia practice contributing to preventable morbidity and mortality. In this literature review, rare and delayed complications following spinal anaesthesia are discussed.
1. Accidental injection of wrong drugs into subarachnoid space
Case report 1:
Intrathecal injection of tranexemic acid(Indian J Anaesth 2012;56:168-70, Mar-Apr 2012)
Accidental injection of tranexemic acid into subarachnoid space of 37 year old lady, ASA PS I posted for cystolithotripsy
Following spinal, patient complained of severe burning pain in both lower limbs, back and gluteal region, and was irritable. Myoclonic movements were noticed in the lower extremities.
Patient was managed with anticonvulsants, intensive haemodynamic monitoring, and CSF lavage. The ampoules of Bupivacaine (5 mg/mL, trade name “Sensovac Heavy”) and tranexamic acid (500 mg/ml, Trade name “Nexamin”) were similar in appearance.
Recovered fully without any neurological sequelae within 1 week
Previous similar reports:
Wong et al. (Ma Zui Xue Za Zhi 1988; 26:249-52) reported the first case of inadvertent intrathecal injection of 75 mg tranexamic acid in an 18-year-old man scheduled for appendicectomy. He developed clonic convulsions that progressed to a generalized seizure, which treated with intravenous diazepam, and the patient recovered without any sequelae.
De leede et al. (J Neurol 1999; 246:843) has reported a case of a 68-yearold man who accidentally received an intrathecal injection of 50 mg. tranexamic acid. Immediately after the injection, he developed status epilepticus. The outcome was complicated, with hypotonic paresis of all four limbs, which resolved but resulted in residual bilateral peroneal palsy.
Yeh et al. (Anesthesiology 2003; 98:270-2) reported that seizures and refractory ventricular fibrillation after accidental intrathecal administration of 500 mg tranexamic acid were associated with fatal outcome.
Case report 2:
Accidental spinal potassium chloride injection successfully treated with spinal lavage (Anaesthesia 2014, 69, 72–76).
A 62-year-old man weighing 75 kg, known hypertensive was scheduled for right total hip replacement under spinal anaesthesia. Ten minutes after injection, there was only patchy blockade, the loss of sensation being inadequate for the planned surgery. Spinal anesthesia was again repeated with the same drug dosage once more. Immediately after the second injection the patient started to complain of severe pain, pruritus, cramps, progressive weakness in both lower limbs (left more than right) and marked sweating. There was complete anaesthesia below the T10 level with hypertension and tachycardia.
Antihypertensive treatment was started. Ten minutes after the second injection, the sensory level had risen to T4; there was flaccid paraplegia with loss of deep tendon reflexes, and pain in both lower limbs. Cerebrospinal fluid lavage was done. Immediately after the lavage, the patient developed signs and symptoms of pulmonary oedema; this required sedation, tracheal intubation and mechanical ventilation.
Eight hours after the lavage, the patient became haemodynamically stable, and started to move his legs and then was extubated. cutaneous sensation had returned to normal. A magnetic resonance scan of both thoracolumbar spine and brain was normal
There were no neurological deficits, and the signs of autonomic hyperactivity had disappeared
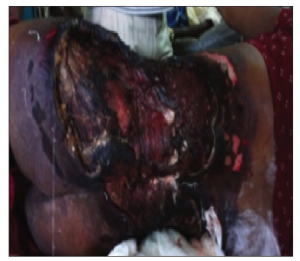
2. Necrotising fascitis
(Indian Journal of Anaesthesia | Vol. 57| Issue 3 | May-Jun 2013)
Case report:
A 27-year-old parturient, ASA I PS received uneventful spinal anaesthesia for caesarean section delivery. Patient was admitted in the emergency department with severe pain, swelling, erythema and blackening involving nearly whole of the back, part of anterior abdomen and gluteal regions accompanied by fever and chills 20 days days following delivery. There was no history of diabetes mellitus, chronic infections, immunosuppressive medications intake and leukemias or lymphomas.
Despite of intensive management of septic shock patient died on third day.
3. Intraspinal and intracranial subarachnoid hemorrhage with severe cerebral vasospasm
Intraspinal combined with cerebral subarachnoid hemorrhage has been rarely reported as a complication after lumbar spinal anaesthesia. Acute intracranial and intraspinal subarachnoid hemorrhage after lumbar puncture is a rare but life threatening complication, requiring urgent diagnosis and therapy.
A 35-yr-old multigravida at 34 week gestation with antenatal history of arterial hypertension and polycystic kidney disease, admitted for forceps delivery under spinal anesthesia.
2 days following spinal anaesthesia, the patient developed severe back pain, headache, vomiting, and stiff neck. Despite analgesia and antiemetic treatment, symptoms increased in intensity, with paraplegia on fifth day postpartum. Computed tomography showed evolving subarachnoid hemorrhage. Spinal magnetic resonance imaging (MRI) showed a late sub acute subarachnoid bleeding between T5 and 10 with mass effect on the spinal cord. A complete T10–11 and partial T9 bilateral decompressive laminectomy was performed to remove subpial clots from a vascular malformation compatible with a spinal angioma. Following surgery patient was conscious and oriented but had lower limb paralysis and hypoesthesia from T6. Antihypertensive therapy for cerebral vasospasm was started. On the third day in PACU, headache and stiff neck increased along with nausea and vomiting. Cranial MRI showed subarachnoid hemorrhage and hemoventricle in both occipital poles. Conservative treatment with calcium antagonists and antihypertensive agents was maintained. On the sixth day, patient suffered a neurological deterioration with paralysis of the upper left limb and impaired consciousness [Glasgow coma scale (GCS) 5] proceeding to sedation, intubation, and assisted ventilation. With transcranial Doppler ultrasound, a severe vasospasm in both middle cerebral arteries (MCAs) appeared. Cerebral arteriography was performed with balloon angioplasty and intra-arterial verapamil, with a partial recovery of right MCA calibre and distal blood flow improvement with complete recovery in left MCA. After resolution of cerebral vasospasm, the patient regained consciousness and could be extubated in the following hours.
Neurological examination showed GCS 15, flaccid unresponsive paraplegia, and hypoesthesia from T6. The patient was discharged to a specialized centre for rehabilitation.
4. Intracranial Sub Dural hematoma
Rev Bras Anestesiol 2012;62:1;88-95
Case report: 48 year old female, ASA 1PS, with urinary incontinence, uneventful spinal anesthesia with 27 G needle.
Symptoms started after 48h with intense headache and other neurological symptoms, which necessitated surgical evacuation after 17 days of conservative management.
Outcome: complete recovery
5. Subdural hygroma
(Anesth Analg 2002;94)
72 year old otherwise healthy female received spinal anaesthesia at L4-5 with whitacre needle 25G uneventfully.
On D2 she had headache not responding to analgesics and was discharged after a week.She was re admitted at 3 weeks with progressive drowsiness and headache.there was no evidence of raised ICP.Investigations showed bilateral subdural hygromas and patient received dexamethasone. An epidural blood patch was performed with autologous blood, 15ml at the same space.
Completely recovered.
6. Cauda Equina syndrome with profound hearing loss
Anesth Anag 2006;102:1863-64)
Case report:33 year old, male,ASA 1 posted for anorectal surgery in lithotomy position, received uneventful spinal anesthesia with 22 G needle with isobaric bupivacaine.
He developed symptoms of cauda equine syndrome and profound hearing loss with 8h of spinal anesthesia, which persisted even after 21 months. Hearing loss was suggestive of cochlear pathology.
A previous study suggested that hearing loss after spinal could be related to needle size (Anesth Analg 1990;70:517-522).Also case reports are available on cauda equina syndrome with both lignocaine and bupivacaine.
7. Foot drop
(Indian J Anaesth 2011;55,Can J Anesth 2005;52,Rev Bras Anestesiol 2014)
Usually unilateral, but occasionally bilateral foot drop cases have been reported in the literature, though the exact mechanism is not known. It can follow otherwise uneventful spinal anesthesia as well
8. Neurological complications following spinal anaesthesia in a patient with congenital absence of lumbar vertebra
(Indian Journal of Anaesthesia 2014;58(4):484-486)
A 25‑year‑old, short stature (130 cm), ASA I PS received uneventful spinal for caesarean delivery. She was admitted to neurosurgical Intensive Care Unit with complaints of inability to move both lower limbs and bladder and bowel incontinence 6 days after delivery. The patient was non‑diabetic and normotensive. Patient had a history of surgery for swelling over lower back in infancy which was present since birth.
Neurological examination revealed complete motor, sensory and autonomic loss of sensation below L2 level with involvement of bladder and bowel. An X‑ray lumbosacral spine and magnetic resonance imaging (MRI) of the spinal cord revealed congenital absence of L3‑5 lumbar vertebrae with low lying spinal cord at L2 level, with myelitis and arachnoiditis. L2 vertebrae were directly fused to the sacrum without any other deformity at that level. A probable diagnosis of chemical myelitis or direct injury to the cords was suspected. Patient was treated conservatively on rest and high doses of steroid (methyl prednisolone) to which she responded partially after 6 weeks in the form of motor recovery. There was no improvement in bladder and bowel function after 2 years.
9. Broken needle
Result of defective construction of needle. The needle breaks at the junction of the hub with the shaft of the needle. Disposable needles are associated with greater risk.
10. Cardiac arrest
It is the most dreaded complication for the anesthesiologist, more so when it occurs in an apparently healthy person. There are several such case reports in literature, main sources being closed insurance claims and retrospective reviews.
During an early review of the Closed Claims Database it was found that few healthy adult patients experienced sudden cardiac arrest while receiving conventionally-managed spinal anesthesia for relatively minor surgery. The outcome in all cases was death or brain damage. Recurrent patterns of presence of a high level of block of T4, the rapid onset of cardiac arrest approximately 30 minutes after the initiation of spinal anesthesia and the presence of apparently stable hemodynamics and respiration preceding sudden deterioration were seen in about half of the cases. Although cardiopulmonary resuscitation was promptly initiated, epinephrine was not administered until an average of 7 minutes had elapsed. These findings suggest that insufficient restoration of peripheral vascular tone – especially in the setting of high sympathetic blockade – may contribute to the severity of cardiac and neurologic outcome. Spinal anesthesia decreases coronary perfusion pressure during CPR to levels below the threshold for successful resuscitation. Administration of exogenous epinephrine or vasopressin helps to achieve critical threshold of perfusion pressure.
In a recent review of high severity injuries associated with regional anesthesia claims in the 1990’s, 30 claims were found in which death occurred. Of these 30 claims, cardiac arrest during central neuraxial block accounted for one-third of cases and was the single largest cause of death. The current literature contains at least 41 well-documented case reports in which a circulatory mechanism – not respiratory depression or lack of vigilance – played the primary role in sudden cardiac arrest during spinal or epidural anesthesia. Vagal factors (traction, movement, pitocin, fear, athletic heart) were often reported in these new cases.
Caplan et all reported in a review of closed insurance claims.14 cases of sudden cardiac arrest in otherwise healthy patients after spinal anaesthesia. Hypoxia and over sedation could be contributing factors.
The incidence of cardiac arrest in different review varies from 0.04-6.5/10000 cases of spinal anaesthesia.
In a multicentre study in Thailand (Regional Anesthesia, Vol 107,No 5 November 2008), 11 cases of cardiac arrest were reported among 40,271 spinal anesthetic, with death as the outcome in more than 90% of cardiac arrests. The patients involved were both obstetric (5 cases) and non obstetric (6cases).Contributing factors included high blockade, blood loss, hypovolemia, lack of ECG monitoring and spinal given by surgeons due to non availability of anesthetists. Neither bradycardia nor fall in saturation was present in all patients.
Role of undiagnosed pathology should always be kept in mind
Coronary artery spasm
(Journal of clinical anaesthesia 1996;8)
42 year, male, ASA I for testicular tumor excision, received spinal anesthesia with tetracaine and dibucaine.
Patient complained of back pain with peritoneal stimulation and had mild hypotension.Inj pentazocine was given without any effect. Subsequently patient developed hypotension and significant ST elevation on ECG without any chest pain. Heart rate was 62/min. He was successfully treated with a dose of ephedrine IV and nitroglycerine infusion resulting in complete and uneventful recovery
Paraplegia after spinal anaesthesia
(Anesth Analg 2006;102)
82 year old patient posted for management of urinary retention due to prostatic hypertrophy. .Had history of hypertension,COPD, hyperplastic thyroid and mild CAD.
Spinal was administered with 25G Quinke needle at L5 S1 space with hyperbaric bupivacaine. Patient developed signs and symptoms of paraplegia below T1 level 36h postoperatively. Imaging ruled out epidural abscess but showed a mass extending from T4 to T6.A CT guided biopsy of the mass showed it to be tubercular granuloma.
Cranial nerve involvement
Incidence varies from none to 5%. Of the disturbances 60% involve sixth nerve, and 30% involve seventh nerve, 10% involve other cranial nerves. Sixth cranial nerve most commonly involved as it has the longest intracranial course and is vulnerable to dynamic changes in the ‘water cushion’ of the CSF.
Visual disturbances
Ischemia of the optic and other ocular muscles is considered the likely cause of most visual disturbances. Causes are low perfusion from systemic hypotension, low ICP from CSF leakage, Gravity traction on the cranial nerves.
Divergent paresis without positional headache
(Anesth Analg 2006;102)
Case report: 64 year old male for prostatectomy for benign hypertrophy of prostate.20G cutting spinal needle and dibucaine local anesthetic were used in otherwise uneventful spinal anesthesia at L4-5.
Patient developed divergent paresis on D17 without evidence of abducent nerve palsy. It was characterized by horizontal diplopia for distant objects, more than 2 meter distance. There was no nystagmus. The condition was thought to be due to CSF hypovolemia as characterized by MRI findings. Absence of positional headache, a characteristic of CSF hypovolemia was unusual in this patient.
Completely recovered by D46.
Epidural abscess
Can result from contamination of epidural space and is due to faulty spinal puncture technique.
Septic meningitis
Can occur due to inadequate sterilization of equipment, bacterial contamination of the anesthetic agents, or the introduction of the spinal needle through the infected tissue.
Meningismus
It is one of the non infective complications due to inflammation of meninges resulting from coming into contact with the chemicals like iodine used for skin preparation. Occurring quite suddenly and usually during third and fourth day, it presents as intense headache, neck stiffness, positive kernig’s sign and photophobia. It is non progressive and subsides with treatment and antibiotics.
Cauda equina syndrome
(BJA 2000; 84 121-6)
Albert Wolley and Cecil Roe became paraplegic following spinal anaesthesia for minor surgery in Chesterfield Royal hospital in 1947. Spinal anaesthesia was given by the same anesthesiologist, with the same drug on the same day in the hospital. The most probable cause of paralysis was an acidic descaler that was allowed to remain in the sterilizing water boiler. The spinal needles and syringes were then boiled in acid which subsequently contaminated the spinal anaesthetic solution when it was withdrawn from the ampoule before injection.
Transient Neurological Symptoms (TNS)
Earlier this condition was called transient radicular irritation. Though traditionally believed to occur with lignocaine intrathecal administration, especially with 5% hyperbaric, it has been described with every local anesthetic. Lignocaine and mepivacaine are more commonly associated with TNS than bupivacaine and could be due to drug per se, dextrose of epinephrine. Symptoms of pain in the buttocks radiating to legs, unilateral or bilateral is most common presentation. Onset is within 24 hours of spinal anaesthesia and spontaneous and complete recovery is the rule. Type of needle also can influence the development of TNS.
Pulmonary embolism
In elderly orthopedic patients with hip fractures, who are often bed ridden, movement of the limb for fracture reduction on the table after spinal anaesthsia, can lead to pulmonary embolism and sudden cardiac arrest (personal experience).This is not directly related to spinal anaesthesia, but occurring immediately after spinal, it has significance for the anaesthesiologist.
Take home messages……….
- Neither healthy patients nor apparently uneventful spinal anesthesia does not totally preclude development of complications.
- Outcome can vary from complete recovery to neurological deficit or death
- Wrong drug administration still continues to occur, with disastrous consequences
- CSF lavage was found to be extremely useful when a wrong drug administration is identified
- All patients should receive aggressive symptomatic and supportive treatment
- Obstetric patients are at higher risk of complications due to spinal anesthesia